About Us
Explore our Simulation Program
Health care simulations have roots in aviation as far back as 1929. The idea of simulation as a health care training tool was adopted in 1968 with a focus on patient safety. Established in 2009, Cook Children's Simulation Program services eight companies within our system with over 10,000 employees.
Who we train
Cook Children's Simulation Program works in collaboration with department educators, leadership teams and multiple committee chairs to support education, training and competency validation along with interprofessional teamwork and team communication supporting the organization's initiative for Zero Harm. Simulation reaches across department and company lines and provides experiential learning for frontline staff: physicians, advanced practice providers, nurses, respiratory therapists, OT, PT, ST, radiology as well as nursing students, medical students, families of our special needs children, chaplains, security, pharmacy and child life specialists. Our simulation lab supports over 20,000 hours of training annually and typically has 10,000 unique learner visits each year.
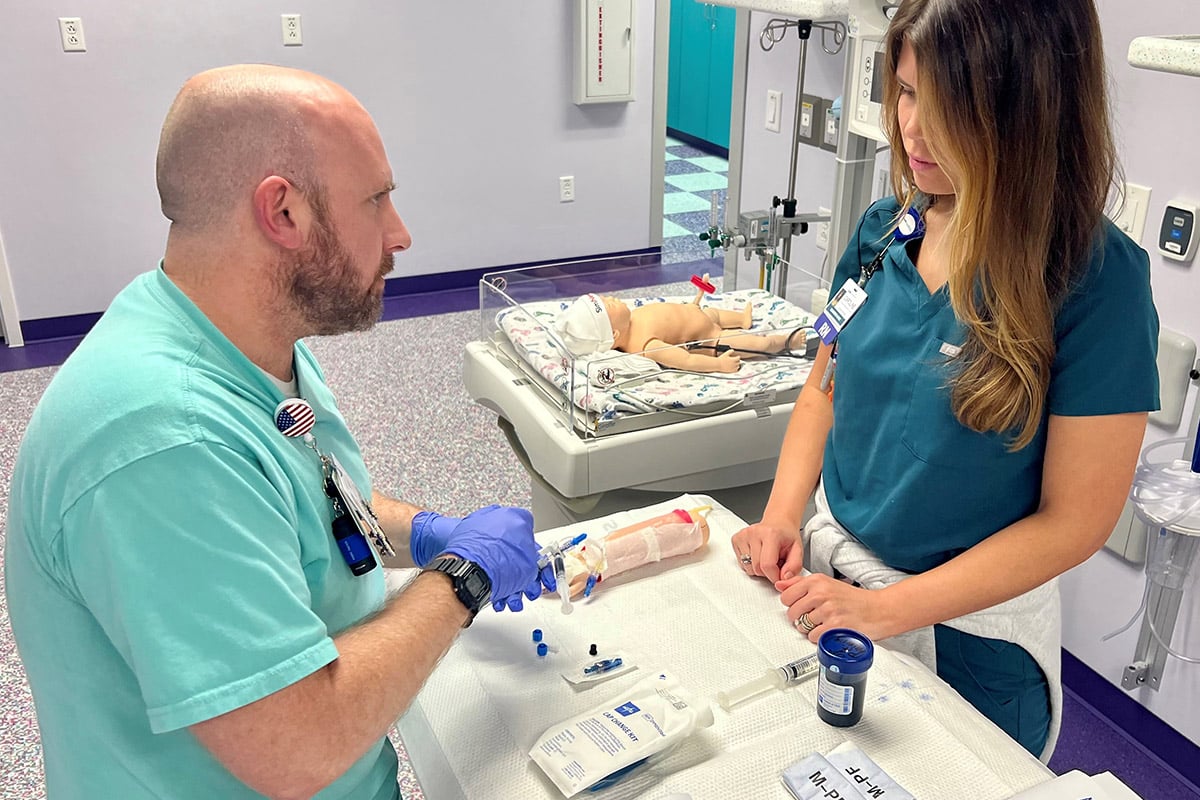
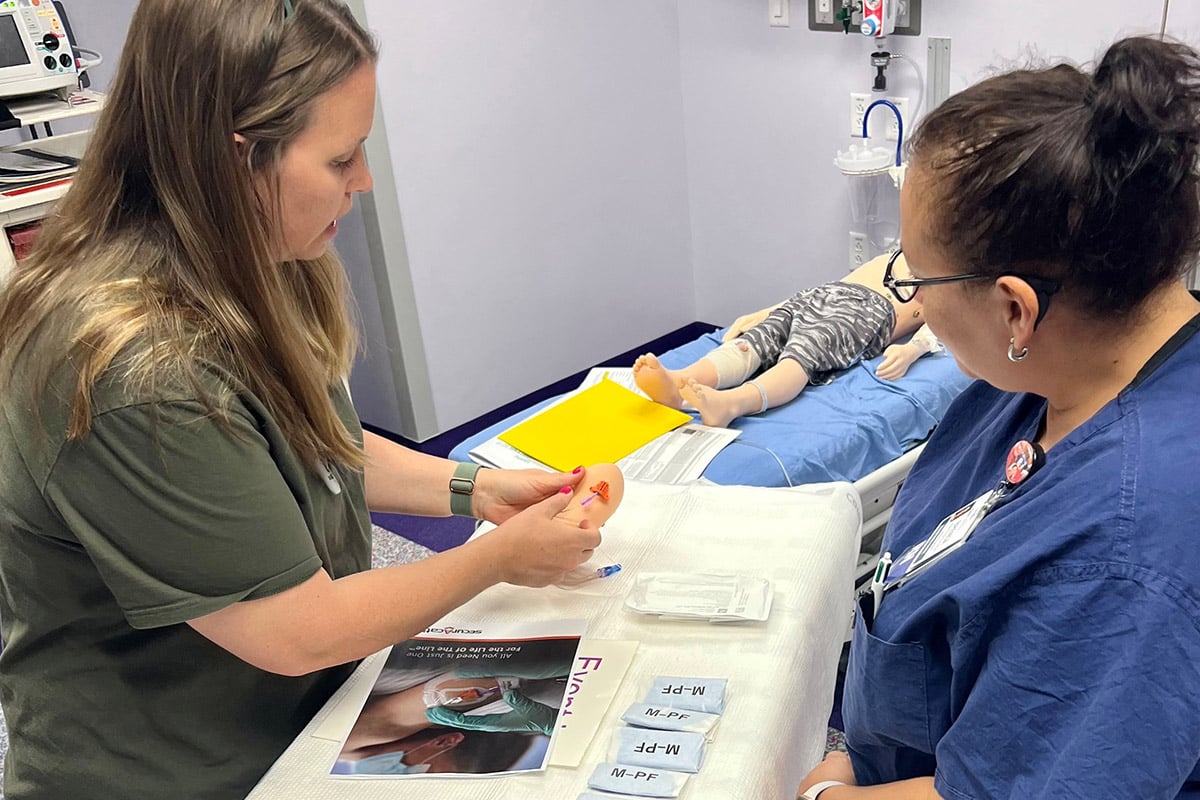
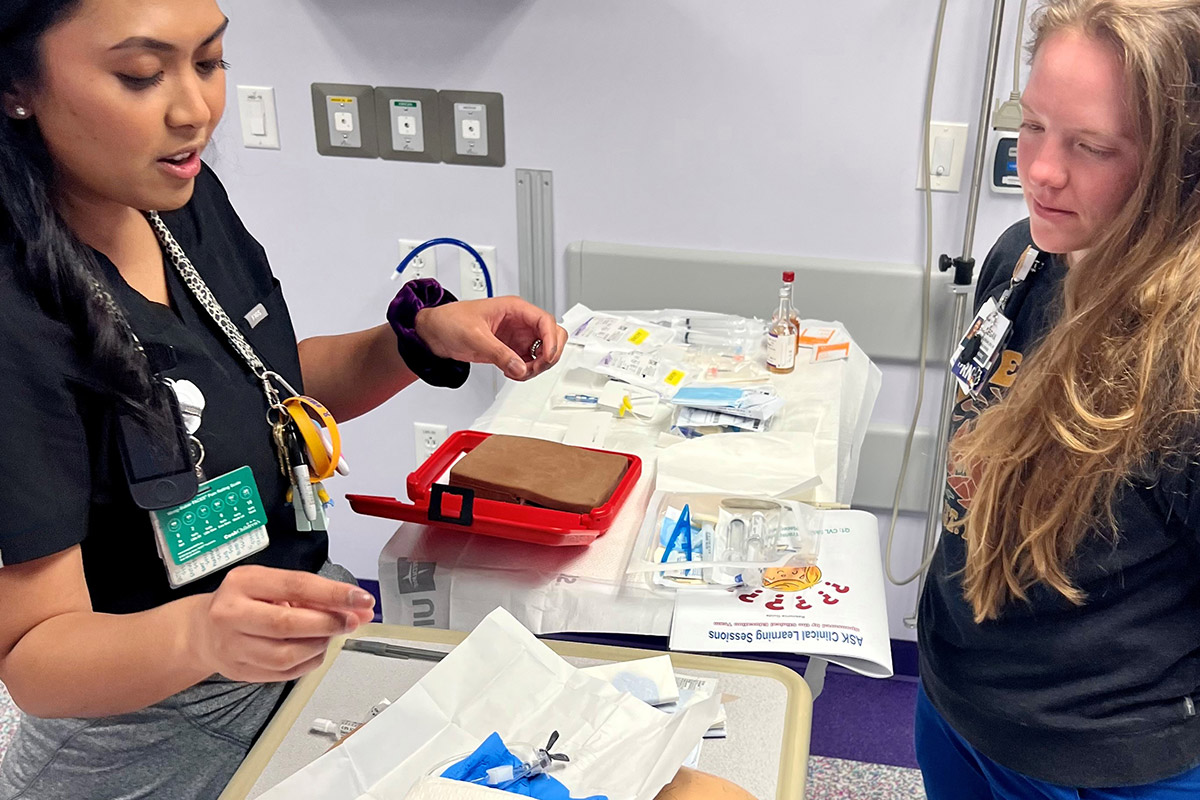
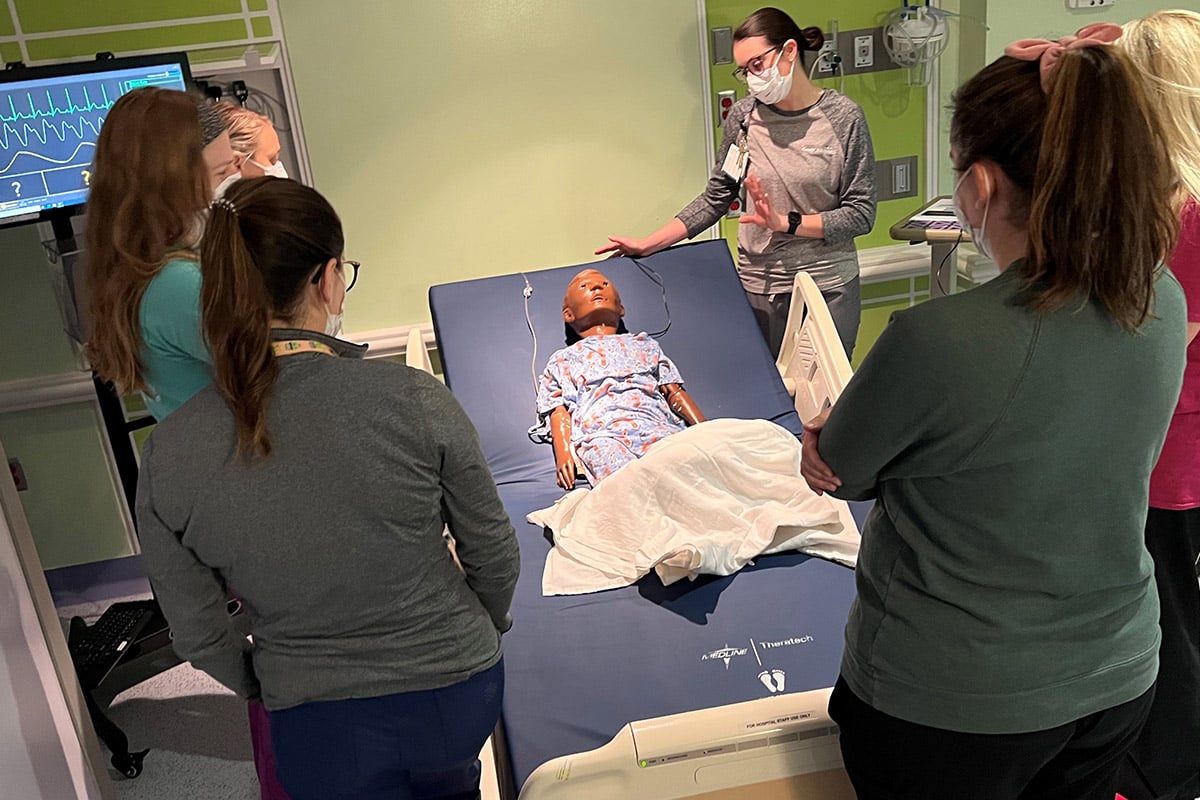
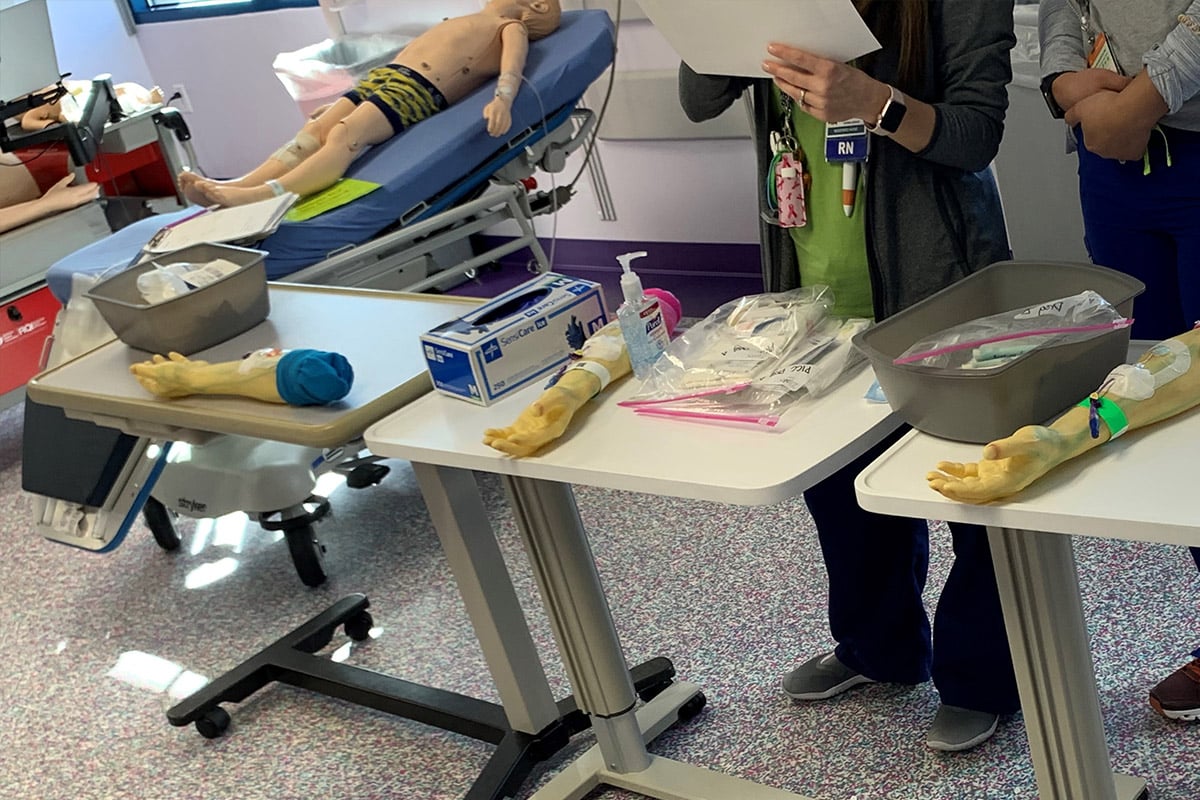
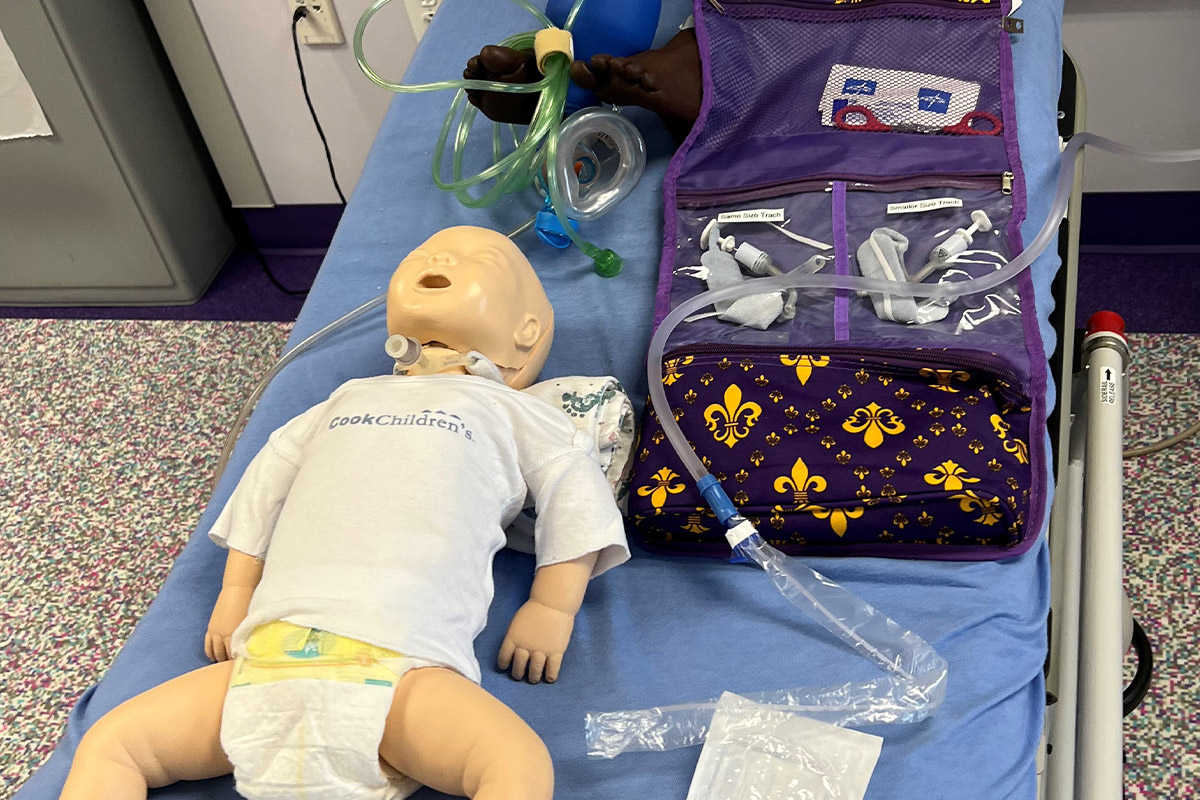
Cook Children's Simulation Program training participants.
How it works
Simulation offers possibilities to learn that extend far beyond the traditional lecture and classroom. This experiential learning allows opportunities to experience new roles, take risks, solve problems, make decisions, practice skills and build communication techniques all in a safe environment that mirrors the workplace. Any type of medical situation, diagnosis, and critical communication scenario can be created, ranging from basic clinical skills to critical care situations like transporting a patient on extracorporeal membrane oxygenation (ECMO).
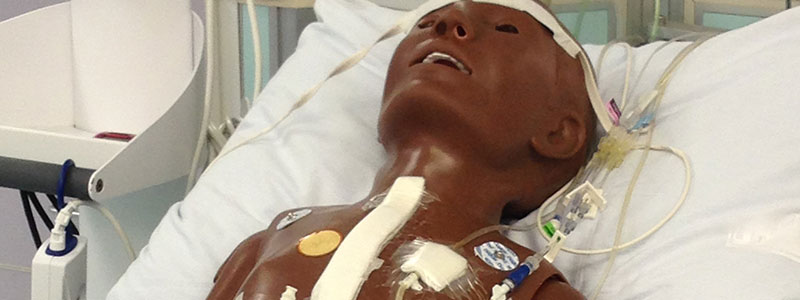
Experiential learning allows the Simulation Program to create realistic situations.
Where is the simulation lab?
Cook Children’s Simulation Lab is now newly named The Louden Family Clinical Learning Center. It is located near downtown Fort Worth, Texas, near the medical center in the 901 7th Ave. building.
Our 2,500 square foot Simulation Lab features 9 open ward bed spaces, 2 isolation rooms, 1 conference room, 2 storage work rooms, and 4 cubicle office spaces. All bed spaces are plumbed with medical gases, providing realistic patient care areas.
Simulation can go "on the road," which is called in situ. With tetherless high-fidelity simulators, we are able to create very specific training and education for our companies, departments, and units. Examples of in-situ simulation include Urgent Care Centers, Child Study Center, Teddy Bear Transport at Meacham Airport, Dodson Specialty Clinics, Emergency Department, Critical Care Units, Surgical Services Departments and various other off-site Cook Children's campuses.

In-situ training encompasses a variety of off-site campuses, such as Teddy Bear Transport.
Our methods and modalities
Over the last ten years, we have increased our fleet of simulators, task trainers, and blended learning technologies. Understanding that the method of simulation has greater value than the modality, our simulation program focuses on developing facilitators who will collaborate with the simulation team to determine which simulator and technology modality best supports the learners and event objectives. Walking through Cook Children's simulation lab, you find the smallest premature baby at 600 grams to a large 200 lb high school football player named "Jack". We have simulators of all ages that talk, cry, turn blue, have seizures, wiggle and have vital signs. The level of fidelity varies and we find that getting back to basics is fundamental. Not only do we have simulators, but we have virtual reality capability, computerized virtual patients, Pediatric Auscultation Trainers, rhythm generators, and task trainers of a wide variety: lumbar puncture, CPR, tracheostomy, G-Button, CAUTI, and IV access, including PIV & central lines, just to mention a few.
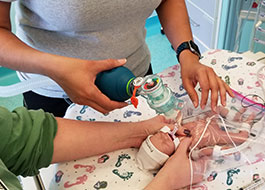 |
 |
 |
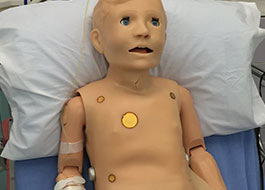
Cook Children's Simulation Lab features realistic simulators, virtual reality capability, computerized virtual patients and a wide variety of task trainers.
Why support our simulation program?
Simulation enables us to prepare our health care staff for the unexpected, train on new equipment, and keep our staff up to date on certifications, evidence-based practices, policies, and procedures. It is invaluable for providing expert training and use in orientation, competency validation, and certifications. Simulation is an excellent evaluation tool to incorporate into applicant interviewing for high-stakes positions like critical care, transport, and emergency medicine.
What staff say about our program
Melissa Gilbreath, a registered nurse that worked in the Cardiovascular Intensive Care Unit, is thankful for the Simulation Program. Melissa underwent extracorporeal membrane oxygenation (ECMO) training in the lab. Having a patient on ECMO at Cook Children's is relatively rare, but Melissa echoed that it is always best to be prepared. The complexity and technicality of the ECMO machine leaves little room for error. She said she practiced with the ECMO machine multiple times in the lab during her orientation and during a practice session. A few days after the practice session, she and her team cared for a patient on ECMO. "I can confidently say I would not have been able to effectively or safely perform that skill if I had not practiced it with my team in the Simulation Lab," Melissa said.
Becky SouthWorth, director of Cook Children's Simulation Program, said she too is thankful for the Simulation Program and all of the learning opportunities it provides for our nurses. "There will always be evidence-based practices that change with science," she said. "As those changes happen, there will always be the need for us to update the way we teach, the equipment we use and the research that we do. The ability to do all of this can be supported with donations. The gifts that come in are used to enhance the lives of future children."
Want to make a difference in the lives of children? Visit cookchildrenspromise.org.
We're here to help.
For more information, please email us at simulationlab@cookchildrens.org