Magnetoencephalography
Basic priniciple of MEG
Magnetoencephalography (MEG) is a non-invasive electrophysiological imaging technique that measures the magnetic fields generated by the human brain. MEG is performed using a magnetometer, a specially designed tool (i.e. coil) that records minute magnetic fields in the range of femto-Tesla (1015) to pico-Tesla (1012). MEG offers an excellent temporal resolution in the range of sub-milliseconds and a very good localization (spatial location) accuracy of a few millimeters, especially for superficial cortical sources.
MEG recordings are based on the phenomenon of electromagnetic induction (also known as Faraday's law) which is a process where a conductor (i.e. pick-up coil) placed in a changing magnetic field causes the production of a voltage across the conductor (Fig. 1, bottom left). The amplitude of this voltage is instantaneously proportional to the magnetic induction’s and readily measurable.
Thousands of active neurons located in a focal area of the human brain are able to produce electrical currents. These currents generate extremely weak magnetic fields, which are measurable outside the human scalp from a magnetometer (Fig. 1, bottom right). The magnetometer is able to convert these weak magnetic field changes into voltage (Fig. 1, top right).
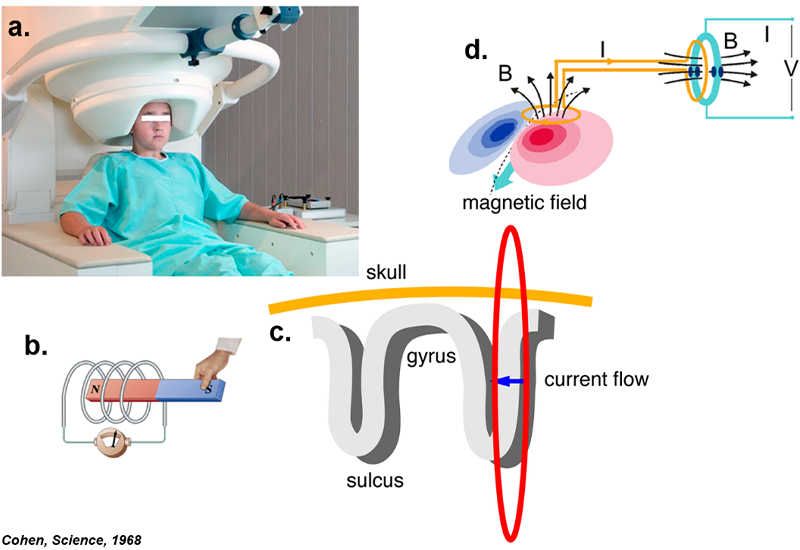
Figure 1: MEG recordings and their principle. Top left: During a MEG recording, the child places his/her head inside a specially designed helmet that accommodates the magnetometers. Top right: MEG recordings are based on the phenomenon of electromagnetic induction according to which any change in the magnetic field can be measured by a nearby coil. Bottom: To generate a MEG signal that is detectable, approximately 50,000 active neurons are needed to be active almost simultaneously. These neurons generated an electric current that produces a magnetic field, which is measurable outside the head with a magnetometer. The magnetometer is sensitive enough to measure this weak activity and convert it to voltage.
Physiology
There are three separate basic neuronal events that are likely candidates to generate a measurable magnetic field (Fig. 2). Out of these three events, the postsynaptic ionic currents flowing in the dendrites during synaptic transmission contributes the most in the generation of the MEG signal. Approximately 50,000 active neurons with similar orientations are needed to reinforce each other in order to generate magnetic fields, that can be measured with MEG outside of the human scalp. Such a configuration can be found at the layer of pyramidal cells (pyramid-shaped neurons that are the primary excitation cells in the cortex), which are situated perpendicular to the cortical surface. Bundles of these neurons that are orientated tangentially to the scalp surface project measurable portions of their magnetic fields outside of the head, and these bundles are typically located in the sulci (grooves at the surface of the brain, Fig. 1, bottom right).
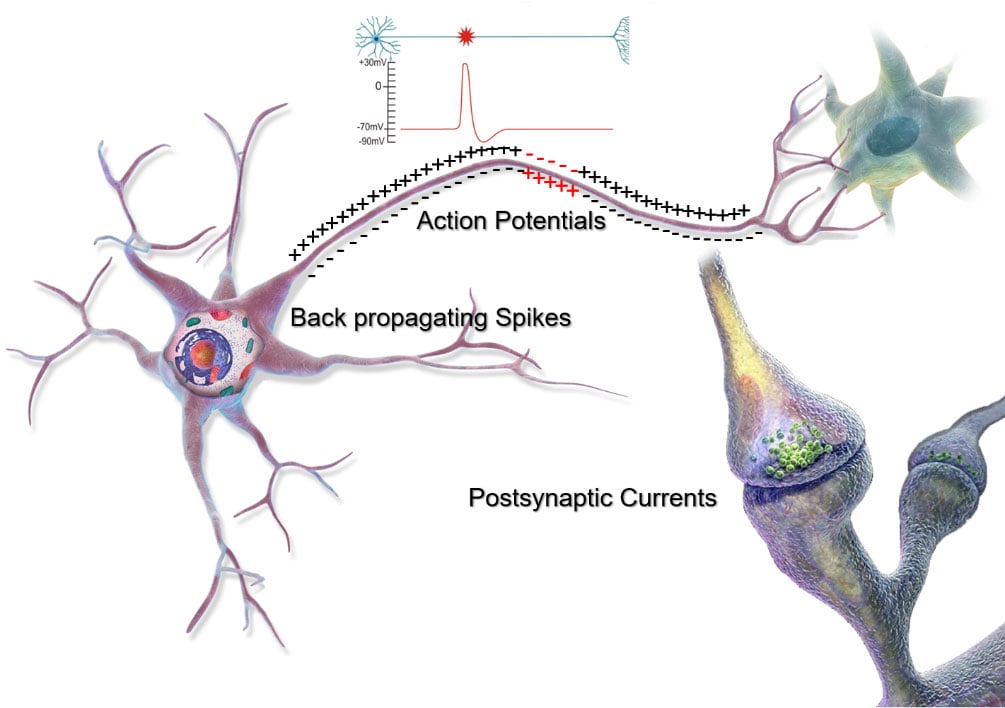
Figure 2: Neuronal events which are likely candidates to generate a measurable magnetic field. Three separate basic neuronal events are likely candidates to generate a measurable magnetic field that can be measured with MEG: (1) action potentials traveling along the axon away from the soma (cell body), (2) postsynaptic currents at the apical dendrites (branched extensions) of neurons, and (3) backpropagating spikes into the dendrites.
According to the equations of Maxwell, any electrical current will produce a magnetic field; it is this field that is measured with the MEG. These magnetic fields are on the order of 10 picoTesla to 10 femtoTesla (1 × 1011 T − 1 × 1014 T). For comparison, the magnetic field of the earth is ~50 microTesla (0.5 × 10-4 T) (Fig. 3). The postsynaptic ionic currents flowing in the dendrites of neurons can be modeled as a current dipole, i.e. a current with a position, orientation, and magnitude, but no spatial extent.
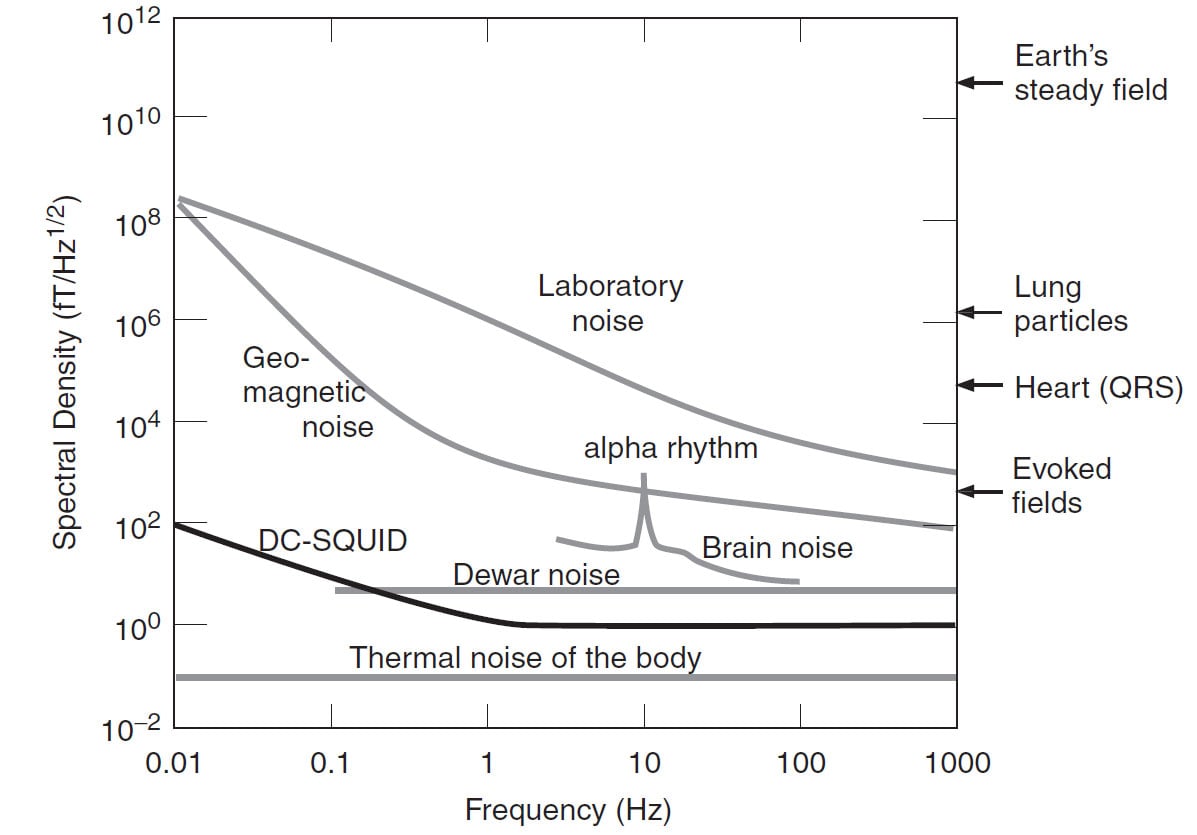
Figure 3: Magnetic field strengths of various sources (adapted from Hämäläinen et al., 1993). Alpha rhythm generated by human brain is several magnitudes lower than the MEG laboratory noise.
Magnetic source imaging
MEG is usually combined with a magnetic resonance imaging (MRI) to get what is called magnetic source imaging (MSI), which offers precise localization of brain activity millisecond by millisecond. MSI is often used in clinical practice for the precise localization of epileptogenic tissue in patients with epilepsy who are unable to control their seizures with seizure medications (Fig. 4). MEG is also used for the localization of eloquent areas (cortical regions that, if removed, result in loss of sensory, language, or motor ability) in the human brain during presurgical mapping. In research, MEG is used to help us understand the function of the human brain and to monitor functional brain plasticity in response to rehabilitation.
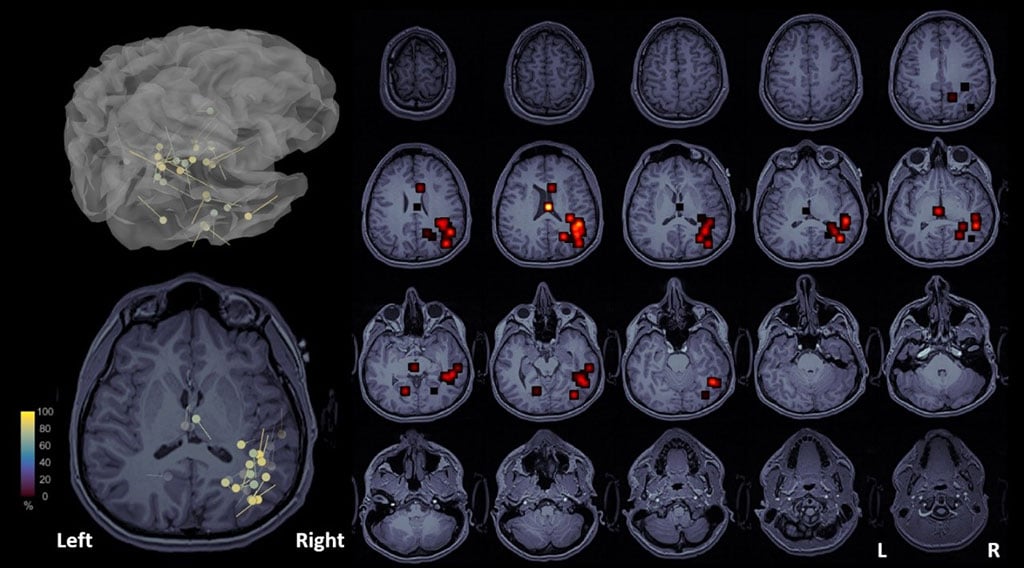
Figure 4: Magnetic source imaging in presurgical evaluation of epilepsy patients. MEG is able to provide the source locations of ictal and interictal activity in children with refractory epilepsy by solving a complex mathematical problem, called inverse problem. The source locations (dipoles) are overlaid on patient’s magnetic resonance imaging (MRI) and create magnetic source images (MSI). Data are from a 16-year-old boy with medically refractory epilepsy. MSI shows a focal epileptogenic source in the right temporo-parietal area.
Equipment
Magnetically shielded room (MSR): Since the magnetic signals emitted by the brain are on the order of a few femtoTeslas, shielding from external magnetic signals is necessary. The shielded room minimize the interference from external electromagnetic sources (i.e. power lines, radiofrequency signals from portable devices, electrical devices and computers, magnetic fields from moving magnetized objects such as cars, elevators and trains, Fig. 3). This magnetic shielding can be obtained by constructing rooms made of aluminum and mu-metal (a nickel–iron soft ferromagnetic alloy with extremely high permeability) for reducing high-frequency and low-frequency noise, respectively (Fig. 5, left). These rooms are called magnetically shielded rooms (MSR); they consist of nested layers each made of pure aluminum and pure mu-metal (Fig. 5, left).

Figure 5: Magnetically Shielded Rooms protect MEG recordings from ambient noise. Left: The MEG system is located inside MSRs, which are made of different layers of aluminum and mu-metal; Right: Elekta Neuromag Triux 306 sensors MEG system at Cook Children’s located inside the MSR.
MEG system: Our lab is equipped with a Triux 306 sensors MEG system (ElektaNeuromag, Helsinki) (Fig. 5, right). Our MEG system records biomagnetic brain activity every millisecond (maximum sampling rate 5 kHz) with an overall sensitivity of 2.3 femtoTesla using 102 magnetometers and 204 planar axial gradiometers. The lab is also endowed with state-of-the-art MEG compatible peripheral devices (i.e. visual, auditory, tactile, and electrical stimulation) and for monitoring high-density electroencephalographic (HD-EEG) activity concurrently with the MEG recordings.
Our magnetometer is located inside an MSR where the recordings are performed. The MSR is equipped with adjustable lighting and an audio-visual communication system that allows communication with the researchers seated outside. Brain activity is measured by positioning the child’s head inside a helmet that contains 306 magnetic field detection coils (102 magnetometers and 204 planar axial gradiometers), which are inductively coupled to very sensitive magnetic field detection devices called superconducting quantum interference devices (SQUIDs). The assembly consisting of a detection coil and a SQUID is made of superconductors, which lose electrical resistivity below a critical temperature, near the temperature (-268.95 °C) of liquid helium. In order to maintain such a low temperature, MEG uses liquid helium that is stored in a specially designed tank. SQUIDs convert the magnetic flux passing through the detection coils into voltage changes. These voltages are recorded in a high performance computer and stored for analysis.
History
MEG signals were first measured by David Cohen in 1968 at the University of Illinois. This first recording was performed inside a MSR using a copper induction coil as the detector (Fig. 6). The coil detector was barely sensitive enough, resulting in poor, noisy MEG measurements that were difficult to use. Later, Cohen built a much better shielded room at MIT, and used one of the first SQUID detectors, just developed by James E. Zimmerman, a researcher at Ford Motor Company, to again measure MEG signals.
At first, a single SQUID detector was used to successively measure the magnetic field at a number of points in succession around the subject's head. This was cumbersome, therefore, in the 1980s, MEG manufacturers began to arrange multiple sensors into arrays to cover a larger area of the head. Present-day MEG arrays are set in a helmet-shaped vacuum flask that typically contains approximately 300 sensors, covering most of the head. In this way, a MEG of a subject or patient’s entire head can now be collected rapidly and efficiently.

Figure 6: David Cohen performed the first MEG recording. Dr. Cohen in front of his shielded room at MIT where the first MEG recording was performed with a SQUID. Lower left inset: the copper induction coil used as detector at the first MEG recording. Below is section of the first MEG recordings using a SQUID showing an alpha brain wave while a healthy subject had their eyes closed.
MEG visit
The child’s preparation is minimal, and the experiment is well tolerated. The entire session lasts about 2–3 hours with the actual measurements lasting around 60 minutes, depending on the study. In some cases, we ask parents to bring the child sleep deprived by either skipping a nap or waking her/him up earlier in the morning, and let the child go to sleep in our facility once the preparation procedure is completed. For research studies, we never use sedation for the recordings.
After completing the consent process, children may change their clothing to a non-metallic hospital gown. We then place specially designed coils on the child’s head, which are used to locate the position of child’s head with respect to the MEG sensors. The child’s head is then digitized with the FASTRAK digitization system, which reconstructs the child’s head shape. The child will be asked to sit on a chair where the FASTRAK transmitter is attached. The FASTRAK receiver is placed securely on patient’s head using specially designed goggles. The researcher then uses the stylus to digitally mark the basic anatomical landmarks on the child’s face and behind their ears (Fig. 7). Beyond the basic anatomical landmarks, additional points are also recorded to provide the best possible localization precision.

Figure 7: Co-registration process with the FASTRAK digitization system. The researcher digitizes anatomical locations of the child’s head using the stylus of the FASTRAK digitization system.
When the child’s preparation finishes, we accompany the child inside the MSR. The child either sits on a comfortable chair or lies down on a bed and places their head inside the MEG helmet (Fig. 8). Parents can monitor their child via a TV screen located outside the MSR. The parent or a research assistant can be in the MSR during the recording. During the experiment, the child can watch their favorite movie on a screen placed in front of them.
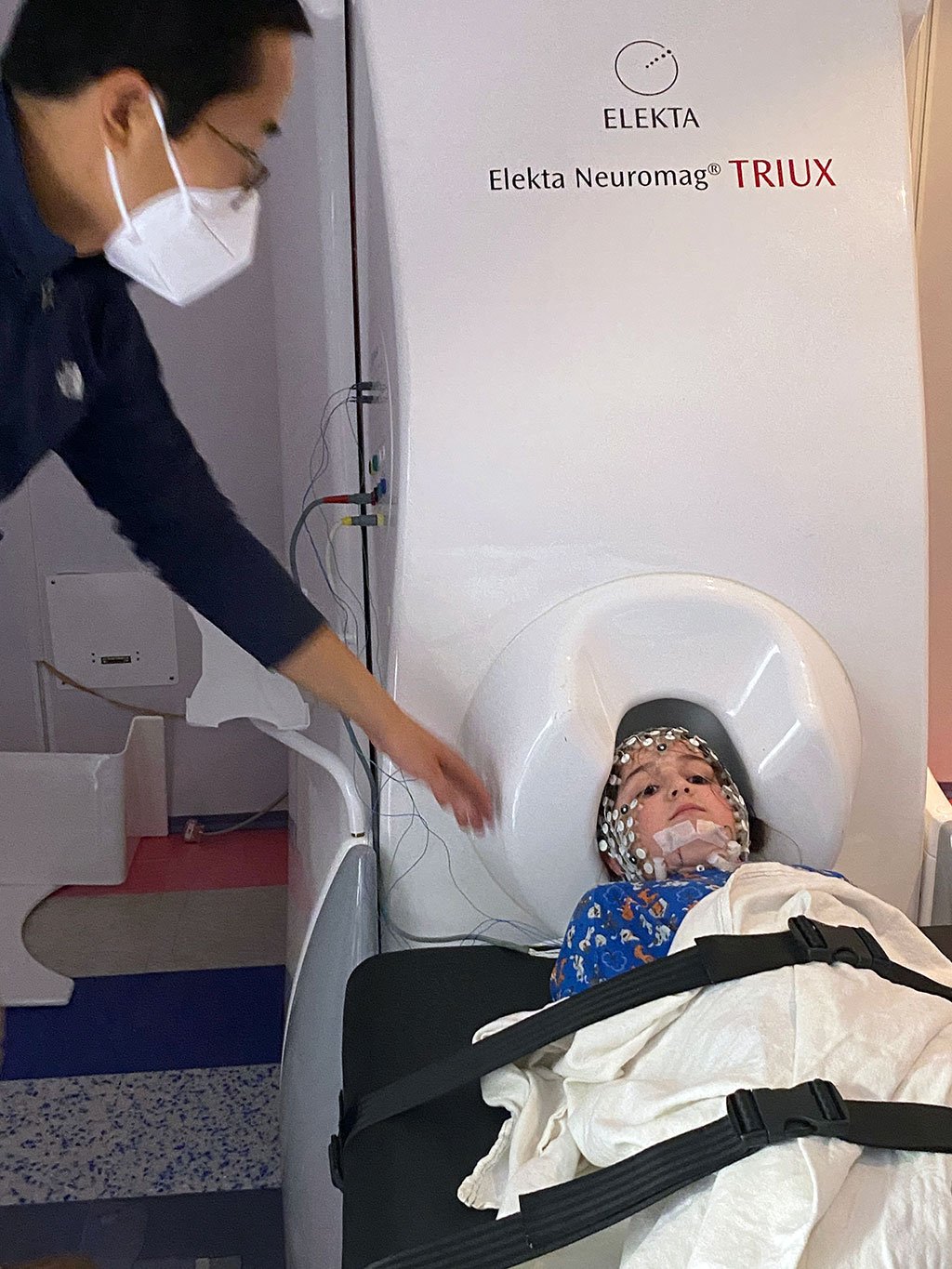
Figure 8: Simultaneous MEG and HD-EEG recordings. The child can either lay down on a specially designed bed (top) or sit in a specially designed chair and watch a screen (bottom) while placing their head inside the MEG helmet that accommodates the gradiometers and magnetometers.
Advantages and limitations of MEG
Compared to other neuroimaging methods, MEG presents a unique set of significant advantages. Compared to electroencephalography (EEG), preparation for a MEG recording is faster and easier. With MEG, the brain activity can be measured immediately after placing the child’s head inside the special helmet since there is no need to attach any sensors to the head. Unlike EEG signals, MEG signals are not distorted by skull conductivity. MEG is also less distorted than EEG by unfused regions of the cranial bone such as fontanel or suture. Moreover, MEG signals are reference free providing absolute measurements of the magnetic field produced by the brain, in contrast to EEG, which provides potential differences between two locations. MEG signals can be measured with a high density of magnetic field sensors. In contrast, EEG always faces the problem of “bridging” between electrodes, meaning a salt bridge is created by the electrolyte/conductive solutions touching each other between electrodes in close proximity to each other. This can occur more often in children or anyone with a smaller head. Both EEG and MEG have excellent temporal resolution and very good spatial resolution (Fig. 9).
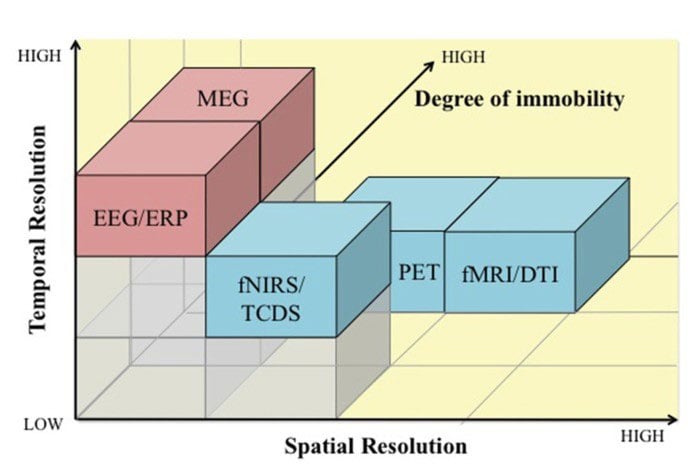
Figure 9: Temporal and spatial resolution and degree of immobility for the different neuroimaging methods. MEG presents excellent temporal resolution and very good spatial resolution compared to other techniques. Adapted from Mehta and Parasuraman (2013).
References
Baillet S. Magnetoencephalography for brain electrophysiology and mapping. Nature Neuroscience 2017; 20(3): 327-339.
Hämäläinen, Matti & Hari, Riitta & Ilmoniemi, Risto J. & Knuutila, Jukka & Lounasmaa, Olli V. 1993. Magnetoencephalography theory, instrumentation, and applications to noninvasive studies of the working human brain. Reviews of Modern Physics. Volume 65, Issue 2. 413-497. ISSN 0034-6861 (printed). DOI: 10.1103/revmodphys.65.413.
Ranjana K. Mehta, Raja Parasuraman. Neuroergonomics: a review of applications to physical and cognitive work. Front Hum Neurosci. 2013; 7: 889. doi: 10.3389/fnhum.2013.00889
Papadelis C, Chen YH. Pediatric Magnetoencephalography in Clinical Practice and Research. Neuroimaging Clinics 2020; 30(2), 239-248
We're here to help
If your child has been diagnosed, you probably have lots of questions. We can help. If you would like to schedule an appointment, refer a patient or speak to our staff, please call our offices at 682-885-2500.